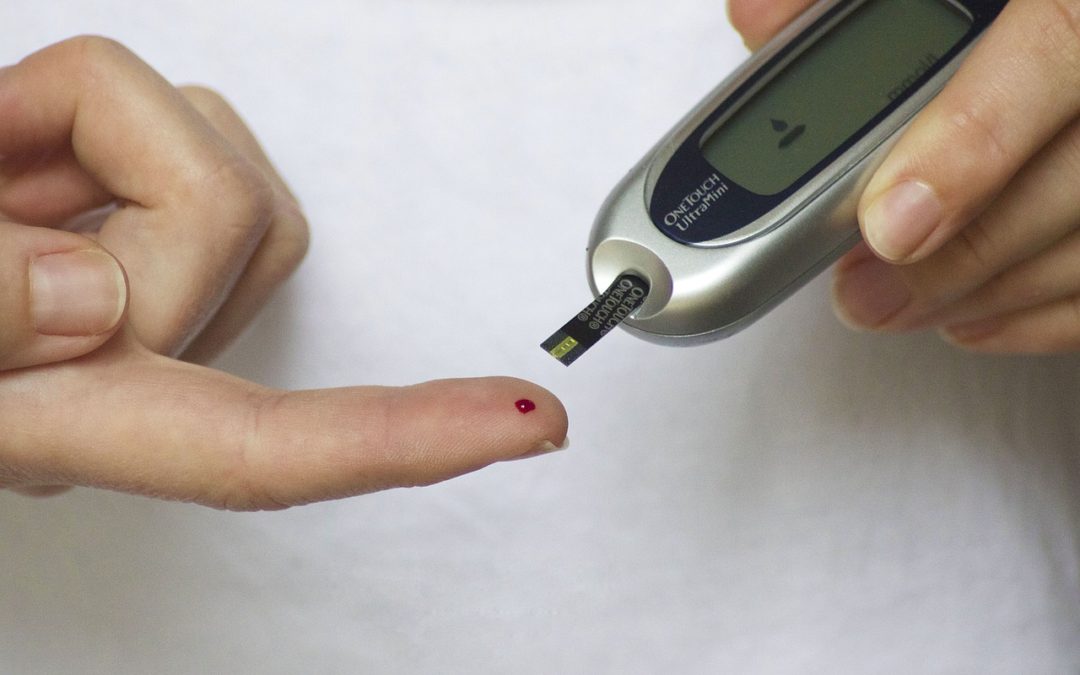
Balancing your blood sugar is one of the most important things you can do for your health. In fact, it's a fundamental pillar in overall health and wellness. This is because imbalanced blood sugar can lead to a host of problems in the body including:
- Stubborn weight gain (especially belly fat)
- Metabolic syndrome including pre-diabetes and diabetes
- Cardiovascular disease
- Alzheimer's disease (read more about why Alzheimer's is now being called “type 3 diabetes” in a published article I wrote here)
- Anxiety, depression and irritability
- Low energy
- Sugar and carb cravings
- Cognitive decline including memory loss
- PMS
- Thyroid problems
- Infertility
- Poorly managed PCOS and HPA axis dysfunction (aka “adrenal fatigue”)
- Headaches
- High blood pressure
- High cholesterol
What we most often associate with blood sugar imbalances is diabetes, a very serious but unfortunately very common disease. In fact, millions of people are likely walking around not knowing they have pre or full-blown diabetes. Dr. Mark Hyman believes that about 90% of people with pre-diabetes or diabetes go unnoticed, mainly because a simple blood test that should be performed by doctors, rarely is. And make no mistake, “pre” diabetes isn't “pre” anything. If you have pre-diabetes you are already at a much higher risk for multiple serious health consequences.
It's not just about blood sugar!
Imbalanced blood sugar levels are one part of the problem but insulin plays a vitally important role as well. What most people don't realize is that insulin actually spikes first before your blood sugar reads in the “danger zone” on blood tests. Insulin spikes first because your body is pumping out more and more insulin to do the job of pushing glucose from your bloodstream into your cells where it's supposed to be used up as energy. This is when we begin to see insulin resistance.
Insulin resistance explained
High carbohydrate meal → increased blood sugar → increased insulin levels → insulin pushes blood sugar into cells where it's supposed to be used as energy
Consistently high carbohydrate intake elevates blood sugar levels. This in turn releases insulin, a hormone responsible for facilitating the transport of blood sugar into cells where it’s supposed to be used up as energy. So in response to raised blood sugar the body releases insulin to shuttle glucose into cells. Insulin resistance occurs when the cells eventually begin to get fed up with the constant onslaught of insulin's yelling at them to open up their doors for glucose. They essentially stop listening to the insulin thereby creating a dangerous state in the body of chronically high insulin and high blood sugar levels. When you become insulin resistant your blood sugar cannot efficiently enter cells to be used as energy and at this point you’ve set yourself up for metabolic dysfunction.
Symptoms of insulin resistance include:
- Fatigue after meals
- Cravings for sweets that don't go away after sweets are eaten
- Increased thirst
- Frequent urination
- Training hard but not losing weight and/or an increase in belly fat or stubborn weight that won’t seem to budge (insulin is our fat storage hormone and blocks fat breakdown)
- Dark pigmentation in the skin folds
- Blood indicators of insulin resistance include: elevated liver enzymes, low levels of HDL cholesterol (“good” cholesterol), a high triglyceride level or a high fasting insulin level
- Irregular menstrual cycles, weight gain, infertility, acne, hair loss or increased facial hair growth (hallmark symptoms of PCOS)
Other issues relating to insulin resistance include:
- Increased activity of aromatase, the enzyme that’s responsible for producing estrogen. This can lead to estrogen dominance, which comes with a whack of issues including certain cancers.
- Increased inflammation in the body
- High blood pressure
- High cholesterol
The insulin and PCOS connection
Polycystic Ovarian Syndrome (PCOS) is a condition in which insulin levels are elevated causing the ovaries to make excessive amounts of androgens by increasing the activity of 12/21 lyase. Additionally, high insulin makes the liver less effective at making sex hormone binding globulin, which is a protein that binds to testosterone keeping it from going haywire and causing excess hair (in unwanted places, such as the face) and pimples: two main symptoms of PCOS. If you have PCOS your risk of type 2 diabetes increases by 80%. Even if you have menstrual irregularities or symptoms of high androgens this increases your risk of type two diabetes by 50%. Read my PCOS cheat sheet here for some tips on how to manage this condition.
How stress can wreak havoc on our blood sugar and insulin levels
Stress → released cortisol → cortisol rises our blood sugar → raised blood sugar stimulates the release of insulin → high insulin causes problems in the body
If you’re under significant amounts of stress this can disrupt your blood sugar balance. This is because when we’re stressed we release cortisol, and one of cortisol’s main roles in the body is to raise blood sugar levels. When cortisol rises so does insulin, (in order to shuttle the glucose released by the cortisol into our cells). This can lead you down the path of insulin resistance as explained above. Anything that raises our cortisol levels be it psychological stress, a parasite infection in the body or food allergies, (which yes, do stress the body out and lead us down this cortisol/blood sugar/insulin path) will raise our blood sugar and thus, insulin. So even if you have the perfect diet, you’re not overweight and you exercise regularly, you can still suffer from blood sugar imbalances and insulin resistance.
Why you need to act NOW and what you can do
High blood sugar can precede the development of type two diabetes by 10 years. And high insulin levels can precede high blood sugar levels for years – even decades – before this. So don’t think you’ve got time to waste. And don't rely on your GP to keep track of whether or not you're entering dangerous territory. Often doctors don't test for elevated insulin levels, instead simply testing fasting blood sugar levels. Unfortunately this does little to prevent problems from arising (remember, insulin spikes first, once blood sugar is high you're already in a dangerous place).
Blood tests are an important tool you can use to prevent and manage high blood sugar or insulin resistance. Other ways you can do this is by employing certain diet and lifestyle strategies. In fact, diet and lifestyle are the best ways to control blood sugar and insulin levels in the body (pssst – even if you're more genetically predisposed to having blood sugar or insulin issues your genes are NOT your fate. Nutrigenomics and epigenetics (the study of how our external environment can affect the expression of our genes) are now showing us that our genes load the gun but diet and lifestyle pull the trigger: you can control the expression of your genes by the diet you eat the lifestyle you lead). Here are some diet and lifestyle strategies that if followed will set you up on a path of optimal blood sugar and insulin control:
- Be mindful of the carbohydrates you’re eating (this includes alcohol, pasta, bread, sugar, juice and soda). Try to eat a low carb, low glycemic index diet.
- Eat a high protein breakfast in the mornings and always consume protein and a healthy fat at every, single meal and snack to slow down blood sugar spikes.
- Consume beans and legumes. Beans have what’s known as the “second meal effect” where they help to stabilize blood sugar levels not only in the meal they’re eaten in but also in subsequent meals – even if they aren’t part of those subsequent meals.
- Consume resistant starch. Resistant starch also has the “second meal effect” just like beans and legumes. It’s not digested in the stomach or small intestines hence the name; because it “resists digestion”. You don’t see spikes in blood sugar or insulin after consuming resistant starch. Examples are cooked then cooled potatoes and rice. However, be sure not to re-heat your resistant starch to over 130 degrees F (54 degrees C). Reheating above this temperature will turn the resistant starch back into digestible starch, which does spike blood sugar levels.
- Take a magnesium bisglycinate supplement. Magnesium is required for proper glucose utilization and insulin signalling.
- Take Chromium picolinate, which reduces insulin resistance. Dietary chromium is poorly absorbed so I recommend you take chromium in supplement form.
- Bump up your omega 3 fatty acids as these enhance the insulin sensitivity of cells. Good sources include chia, hemp, flax, cold water fatty fish or fish or algae oil supplementation.
- Reduce your stress both mental and physical from such things as food sensitivities.
- Avoid dairy: it elicits a high insulin response in the body.
- Moderate exercise increases the body’s sensitivity to insulin so be sure to make exercise part of your daily routine. Be careful though: over-doing it can have the opposite effect: high intensity exercise can raise cortisol levels too much which in turn can raise insulin levels too much. In this instance insulin, being our fat-storage hormone, will hold onto fat instead of releasing it.